/* LOADER */
.ml-form-embedSubmitLoad {
display: inline-block;
width: 20px;
height: 20px;
}
.ml-form-embedSubmitLoad:after {
content: " ";
display: block;
width: 11px;
height: 11px;
margin: 1px;
border-radius: 50%;
border: 4px solid #fff;
border-color: #ffffff #ffffff #ffffff transparent;
animation: ml-form-embedSubmitLoad 1.2s linear infinite;
}
@keyframes ml-form-embedSubmitLoad {
0% {
transform: rotate(0deg);
}
100% {
transform: rotate(360deg);
}
}
#mlb2-957692.ml-form-embedContainer {
box-sizing: border-box;
display: table;
height: 100%;
margin: 0 auto;
position: static;
width: 100% !important;
}
#mlb2-957692.ml-form-embedContainer h4,
#mlb2-957692.ml-form-embedContainer p,
#mlb2-957692.ml-form-embedContainer span,
#mlb2-957692.ml-form-embedContainer button {
text-transform: none !important;
letter-spacing: normal !important;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper {
background-color: #f6f6f6;
border-width: 0px;
border-color: #e6e6e6;
border-radius: 4px;
border-style: solid;
box-sizing: border-box;
display: inline-block !important;
margin: 0;
padding: 0;
position: relative;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper.embedPopup,
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper.embedDefault { width: 400px; }
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper.embedForm { max-width: 400px; width: 100%; }
#mlb2-957692.ml-form-embedContainer .ml-form-align-left { text-align: left; }
#mlb2-957692.ml-form-embedContainer .ml-form-align-center { text-align: center; }
#mlb2-957692.ml-form-embedContainer .ml-form-align-default { display: table-cell !important; vertical-align: middle !important; text-align: center !important; }
#mlb2-957692.ml-form-embedContainer .ml-form-align-right { text-align: right; }
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedHeader img {
border-top-left-radius: 4px;
border-top-right-radius: 4px;
height: auto;
width: 100%;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody,
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-successBody {
padding: 20px 20px 0 20px;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody.ml-form-embedBodyHorizontal {
padding-bottom: 0;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-embedContent,
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-successBody .ml-form-successContent {
margin: 0 0 20px 0;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-embedContent h4,
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-successBody .ml-form-successContent h4 {
color: #000000;
font-family: 'Open Sans', Arial, Helvetica, sans-serif;
font-size: 30px;
font-weight: 400;
margin: 0 0 10px 0;
text-align: left;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-embedContent p,
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-successBody .ml-form-successContent p {
color: #000000;
font-family: 'Open Sans', Arial, Helvetica, sans-serif;
font-size: 14px;
font-weight: 400;
margin: 0 0 10px 0;
text-align: left;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-embedContent ul,
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-embedContent ol,
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-successBody .ml-form-successContent ul,
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-successBody .ml-form-successContent ol {
color: #000000;
font-family: 'Open Sans', Arial, Helvetica, sans-serif;
font-size: 14px;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-embedContent p a,
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-successBody .ml-form-successContent p a {
color: #000000;
text-decoration: underline;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-embedContent p:last-child,
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-successBody .ml-form-successContent p:last-child {
margin: 0;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody form {
margin: 0;
width: 100%;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-formContent,
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-checkboxRow {
margin: 0 0 20px 0;
width: 100%;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-formContent.horozintalForm {
margin: 0;
padding: 0 0 20px 0;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-fieldRow {
margin: 0 0 10px 0;
width: 100%;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-fieldRow.ml-last-item {
margin: 0;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-fieldRow.ml-formfieldHorizintal {
margin: 0;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-fieldRow input {
background-color: #ffffff;
color: #333333;
border-color: #cccccc;
border-radius: 4px;
border-style: solid;
border-width: 1px;
font-size: 14px;
line-height: 20px;
padding: 10px 10px;
width: 100%;
box-sizing: border-box;
max-width: 100%;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-fieldRow input::-webkit-input-placeholder { color: #333333; }
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-fieldRow input::-moz-placeholder { color: #333333; }
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-fieldRow input:-ms-input-placeholder { color: #333333; }
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-fieldRow input:-moz-placeholder { color: #333333; }
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-horizontalRow {
height: 42px;
}
.ml-form-formContent.horozintalForm .ml-form-horizontalRow .ml-input-horizontal { width: 70%; float: left; }
.ml-form-formContent.horozintalForm .ml-form-horizontalRow .ml-button-horizontal { width: 30%; float: left; }
.ml-form-formContent.horozintalForm .ml-form-horizontalRow .horizontal-fields { box-sizing: border-box; float: left; padding-right: 10px; }
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-horizontalRow input {
background-color: #ffffff;
color: #333333;
border-color: #cccccc;
border-radius: 4px;
border-style: solid;
border-width: 1px;
font-size: 14px;
line-height: 20px;
padding: 10px 10px;
width: 100%;
box-sizing: border-box;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-horizontalRow button {
background-color: #000000;
border-color: #000000;
border-style: solid;
border-width: 1px;
border-radius: 4px;
box-shadow: none;
color: #ffffff !important;
font-family: 'Open Sans', Arial, Helvetica, sans-serif;
font-size: 14px !important;
font-weight: 700;
line-height: 20px;
padding: 10px !important;
width: 100%;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-horizontalRow button:hover {
background-color: #333333;
border-color: #333333;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-checkboxRow input[type="checkbox"] {
display: inline-block;
float: left;
margin: 1px 0 0 0;
opacity: 1;
visibility: visible;
appearance: checkbox !important;
-moz-appearance: checkbox !important;
-webkit-appearance: checkbox !important;
position: relative;
height: 14px;
width: 14px;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-checkboxRow .label-description {
color: #000000;
display: block;
font-family: 'Open Sans', Arial, Helvetica, sans-serif;
font-size: 12px;
text-align: left;
padding-left: 25px;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-checkboxRow label {
font-weight: normal;
margin: 0;
padding: 0;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-checkboxRow label a {
color: #000000;
text-decoration: underline;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-checkboxRow label p {
color: #000000 !important;
font-family: 'Open Sans', Arial, Helvetica, sans-serif !important;
font-size: 12px !important;
line-height: 18px !important;
margin: 0 5px 0 0;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-checkboxRow label p:first-letter {
color: #000000 !important;
font-family: 'Open Sans', Arial, Helvetica, sans-serif !important;
font-size: 12px !important;
font-weight: normal !important;
line-height: 18px !important;
padding: 0 !important;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-checkboxRow label p:last-child {
margin: 0;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-embedSubmit {
margin: 0 0 20px 0;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-embedSubmit button {
background-color: #000000;
border: none;
border-radius: 4px;
box-shadow: none;
color: #ffffff !important;
font-family: 'Open Sans', Arial, Helvetica, sans-serif;
font-size: 14px !important;
font-weight: 700;
line-height: 20px;
padding: 10px !important;
width: 100%;
box-sizing: border-box;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-embedSubmit button:hover {
background-color: #333333;
}
.ml-subscribe-close {
width: 30px;
height: 30px;
background: url(https://bucket.mlcdn.com/images/default/modal_close.png) no-repeat;
background-size: 30px;
cursor: pointer;
margin-top: -10px;
margin-right: -10px;
position: absolute;
top: 0;
right: 0;
}
.ml-error input {
background: url(https://bucket.mlcdn.com/images/default/error-icon.png) 98% center no-repeat #ffffff !important;
background-size: 24px 24px !important;
}
.ml-error .label-description {
color: #ff0000 !important;
}
.ml-error .label-description p {
color: #ff0000 !important;
}
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-checkboxRow.ml-error .label-description p,
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-checkboxRow.ml-error .label-description p:first-letter {
color: #ff0000 !important;
}
@media only screen and (max-width: 400px){
.ml-form-embedWrapper.embedDefault, .ml-form-embedWrapper.embedPopup { width: 100%!important; }
.ml-form-formContent.horozintalForm { float: left!important; }
.ml-form-formContent.horozintalForm .ml-form-horizontalRow { height: auto!important; width: 100%!important; float: left!important; }
.ml-form-formContent.horozintalForm .ml-form-horizontalRow .ml-input-horizontal { width: 100%!important; }
.ml-form-formContent.horozintalForm .ml-form-horizontalRow .ml-input-horizontal > div { padding-right: 0px!important; padding-bottom: 10px; }
.ml-form-formContent.horozintalForm .ml-button-horizontal { width: 100%!important; }
}
.ml-mobileButton-horizontal { display: none; }
.ml-mobileButton-horizontal button {
background-color: #000000;
border-color: #000000;
border-style: solid;
border-width: 1px;
border-radius: 4px;
box-shadow: none;
color: #ffffff !important;
font-family: 'Open Sans', Arial, Helvetica, sans-serif;
font-size: 14px !important;
font-weight: 700;
line-height: 20px;
padding: 10px !important;
width: 100%;
}
@media only screen and (max-width: 400px) {
#mlb2-957692.ml-form-embedContainer .ml-form-embedWrapper .ml-form-embedBody .ml-form-formContent.horozintalForm {
padding: 0 0 10px 0 !important;
}
.ml-hide-horizontal { display: none !important; }
.ml-mobileButton-horizontal { display: block !important; margin-bottom: 20px; }
.ml-form-formContent.horozintalForm .ml-form-horizontalRow .ml-input-horizontal > div { padding-bottom: 0px !important; }
}
@media only screen and (max-width: 400px) {
.ml-form-formContent.horozintalForm .ml-form-horizontalRow .horizontal-fields {
margin-bottom: 10px !important;
width: 100% !important;
}
}
function ml_webform_success_957692() {
var $ = ml_jQuery || jQuery;
$('.ml-subscribe-form-957692 .row-success').show();
$('.ml-subscribe-form-957692 .row-form').hide();
}
A cardiac arrest occurs when the victim’s heart stops pumping blood around the body. This causes the victim to become unresponsive and stop breathing. In this CPR blog post, we’ll take a closer look at how defibrillation can help during a cardiac arrest.
A fit heart pumps rhythmically, the heart muscle is controlled by electrical impulses generated within the heart. During a cardiac arrest, this rhythm becomes disorganized or even stops altogether resulting in two broad categories of cardiac arrest:
Shockable rhythms – disorganized electrical activity but no blood being pumped around the body
Non-shockable rhythms – either asystole (no electrical activity) or pulseless electrical activity (electrical activity, but no blood being pumped around the body)
When the heart is in ventricular fibrillation (VF), normal activity may be restored by applying an electric shock with a defibrillator. This process is called defibrillation .
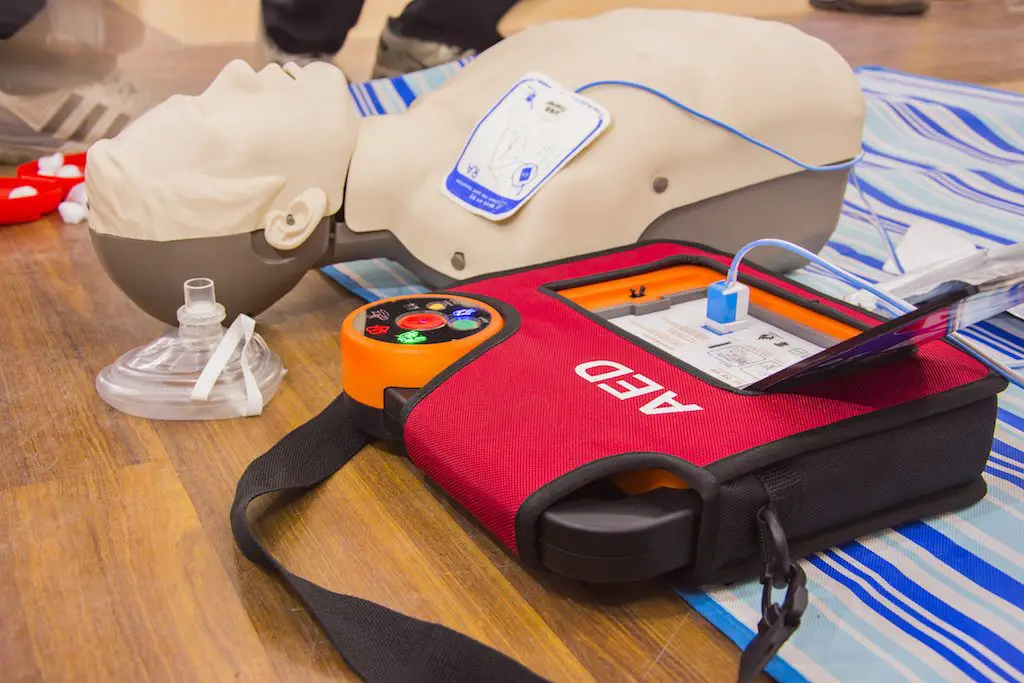
Automated External Defibrillators (AEDs) are devices that are reliable and simple to operate. When attached to the patient’s chest, AEDs analyze the heart rhythm and advise the rescuer on the action to be taken.
An AED being used during CPR training If an AED detects a shockable rhythm such as ventricular fibrillation it will guide the rescuer through delivering an electrical shock.
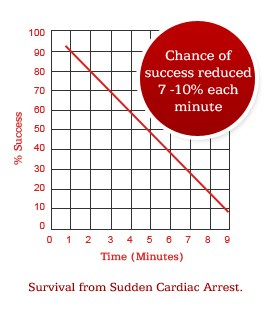
The sooner defibrillation is delivered, the more effective it is. The chances of successful defibrillation decline at a rate of 7 – 10% per minute with each minute of delay following a cardiac arrest.
The chance of success with an AED is improved if effective cardiopulmonary resuscitation has been given to the victim. CPR alone is unlikely to convert ventricular fibrillation into a normal rhythm, however a defibrillation attempt is more likely to be successful if effective CPR has been performed.
AEDs are designed to be used by members of the public with no formal training . However, a trained rescuer is likely to be more confident using an AED and more able to perform high-quality CPR.





good stuf
Thank you!
Kind regards,
John & the team